Take a patient-centred approach to treating cataracts, says NICE.
27 October 2017

The decision to have cataract surgery should be based on whether the patient thinks surgery is right for them, says NICE in new guidance.
The guideline provides advice for patients and ophthalmologists to help them decide when surgery is appropriate, taking into account how the condition is affecting a patient’s sight and their quality of life, the benefits and harms of the operation.
The guideline also says that a decision on whether to offer second-eye cataract surgery should use the same criteria.
Cataracts are a common eye problem where the lens in your eye becomes cloudy. It can affect one or both eyes. They cause blurry, misty vision and sight loss.
It most commonly affects adults as a result of ageing but may also occur as a result of:
- hereditary factors
- trauma
- inflammation
- metabolic or nutritional disorders
- exposure to radiation
- lifestyle factors such as tobacco smoking or a high alcohol intake
Cataracts can be treated by replacing the cloudy lens with an artificial one. This type of surgery is the most common procedure done in the NHS and has a high success rate in improving visual function.
"This is a condition which can severely impair a person’s vision and can lead to a decreased quality of life as daily tasks such as driving or going to the shops seem impossible. This guideline aims to ensure everyone with a cataract has access to timely, sight-restoring surgery.”

The guideline makes recommendations to minimise complications and surgical errors, such as implanting the wrong lens. This includes making sure the correct eye to be operated on is clearly marked and ensuring there is only one lens in the operating theatre.
In adults with early age-related cataracts, non-surgical management may include prescription of spectacles. Currently there are no medicines or eye drops that can be used to treat cataracts meaning surgery is the only long term solution.
“The day I arrived for surgery I was a bit apprehensive but I can say I have had more discomfort from dirt and dust in my eye than the delicate fingers of my surgeon.
"In my opinion this is a life-changing operation. At the start of my cataract journey I didn't expect the results I have experienced."
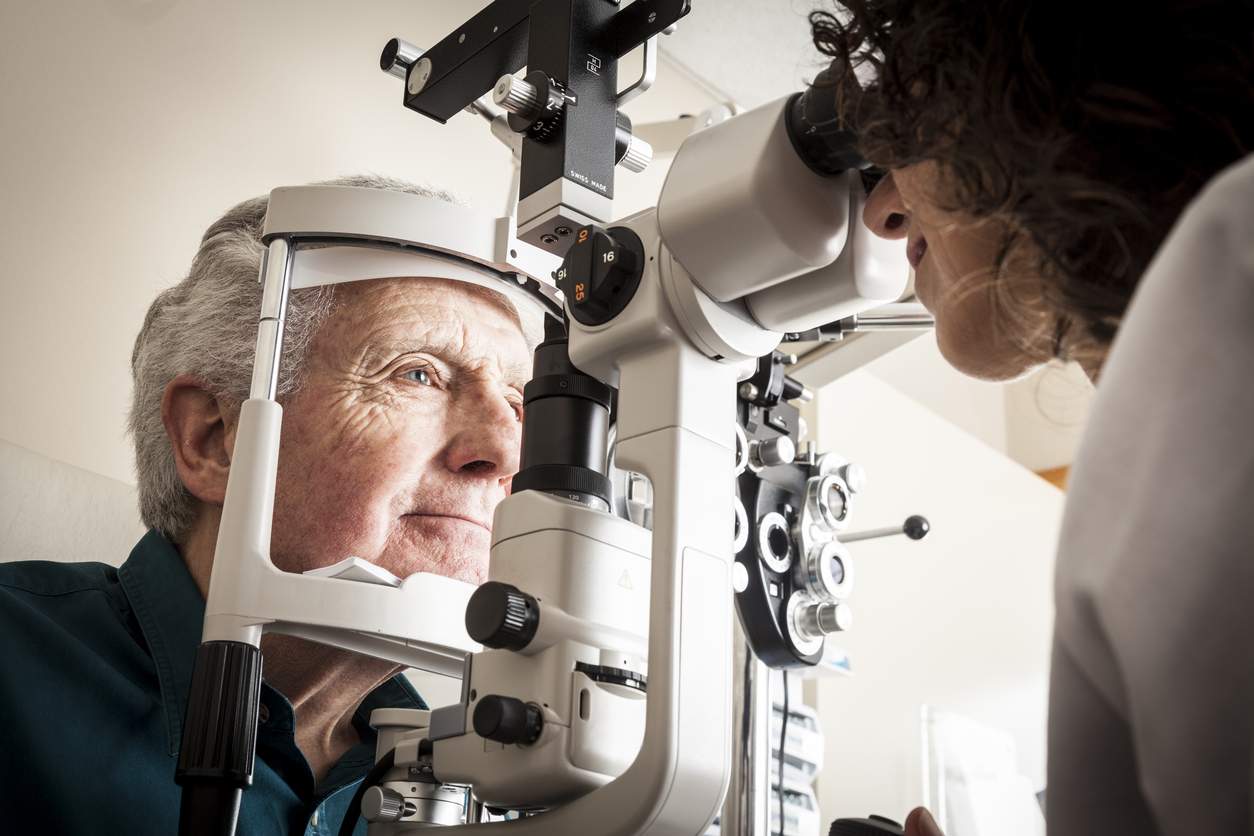
The guidance highlights the importance of providing people with cataracts and their family members or carers, information about the condition and treatment options in a format that is easy for them to understand.
This includes details such as what cataract surgery involves, how long it takes and likely recovery time. It says that patients should be made aware of how their vision and quality of like may be affected without surgery.
“Having had cataract surgery myself I was pleased to be part of the group which developed this important guideline.
"As I know from my own experience, undergoing cataract surgery can be a daunting prospect. Receiving the right advice and support is important to put patients at ease.
"This guideline will be an important tool in ensuring that both patients and clinicians are aware of the standards of care to which the health service should be working."
“Cataract surgery is one of the ways in which the NHS can transform our lives. Our guideline will help patients with cataracts and those treating them to make choices about the treatment they should have.
“We are asking NHS organisations to compare their current practice with our recommendations and to consider what changes may need to be made, to put them into practice. In considering any changes, they will need to take into account any extra costs they may incur. The speed at which these recommendations are adopted by local NHS services will depend on the resources they have available and the other priorities they are dealing with.”

